Menopause: Treatment Options and the Role of Physio
- Caitlin Broger & Jenni Davies
- 1 day ago
- 6 min read
You’ve heard of the "Big Three"—hot flushes, night sweats, and brain fog - but the transition through menopause is about so much more than a portable fan and a lost set of keys. There are many other symptoms that can also occur such as insomnia, muscle and joint aches, anxiety, mood swings, fatigue, vaginal dryness, weight gain, night sweats, dry skin, hair thinning, urinary urgency and/or incontinence.
What Exactly is Menopause?
Menopause: Technically, menopause is a single date on the calendar: the 12-month anniversary of your very last period.
Peri-menopause: This is the "hormonal chaos" leading up to menopause. It can last anywhere from 1 to 10 years, meaning women as young as 35 can start having symptoms.
Post-menopause: Everything following the 12-month milestone of menopause.
Charts of the Hormonal Changes that occur during our Hormonal Lifecycle
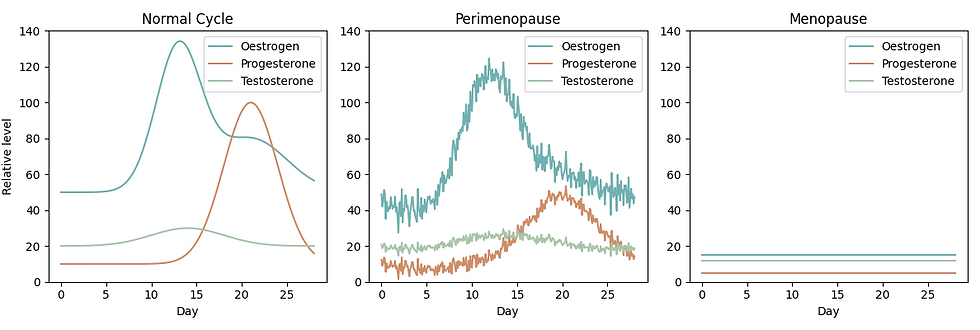
5 Fast Facts: How Menopause Impacts Your Whole Body
Recent research from the APA Women’s, Men’s and Pelvic Health group (2025) highlights that oestrogen acts like a "master key" for your health. When it declines, it triggers a cascade of changes:
1. Accelerated Muscle Loss: Menopause is associated with a significant decline in oestrogen, contributing to an accelerated loss of skeletal muscle mass. Women may lose up to 1–1.5% of muscle mass per year during the transition, which is linked to a decreased metabolic rate and increased heart health risks (El Khoudary et al., 2020). In terms of pelvic health, this may lead to urinary or faecal incontinence symptoms.
2. Increased Fracture Risk: In the 5 to 7 years following menopause, women may lose up to 20% of their bone mineral density. This significantly increases the risk of osteoporotic fractures, commonly affecting the spine, hip, and wrist (National Institutes of Health, 2023).
3. The "Musculoskeletal Syndrome" of Menopause: Over 70% of women experience joint stiffness or "achy" connective tissues. Oestrogen maintains the flexibility and hydration of tendons and ligaments; when it drops, collagen production reduces, leading to lower tensile strength and a higher risk of tendinopathies (Wright et al., 2024).
4. Mental Health & "Brain Fog": Hormonal fluctuations contribute to sleep disturbances, anxiety, and cognitive symptoms. Sleep disruption can actually increase your pain sensitivity and reduce your exercise tolerance (Saghafi et al., 2021).
5. Genitourinary Symptoms (GSM): Up to 70% of postmenopausal women are affected by Genitourinary Syndrome of Menopause (GSM). This describes structural and functional changes in the genitals and urinary tract caused by low oestrogen (Gandhi et al., 2016) which can cause symptoms such as vaginal dryness, burning, urinary urgency, and recurrent UTIs.
Topical oestrogen, otherwise known as vaginal oestrogen, either in an ointment or pessary (tablet) form is a localised form of hormone replacement therapy that can be prescribed by your GP or Specialist.
Is it Safe? Topical vaginal oestrogen (creams, pessaries, or rings) stays local to the vaginal tissues with very little systemic absorption. Current evidence suggests that topical oestrogen is a safe and effective option, even for those who prefer to avoid systemic or traditional hormone therapy (Rueda et al., 2017).
UTI Prevention: Low-dose topical oestrogen can reduce the risk of recurrent UTIs by over 50% (USANZ, 2024).
The Best Results: Recent research suggests that Pelvic Floor Muscle Training (PFMT) combined with topical oestrogen is more effective for tissue elasticity and sexual function than using oestrogen alone (Mercier et al., 2023).

Pelvic Health Physiotherapy and Menopause
Specific pelvic symptoms of menopause, such as urinary or faecal incontinence, urinary urgency, and pain with sexual intercourse, respond really well to Pelvic Health Physiotherapy
Another aspect of pelvic health that can become prominent throughout this whole period is pelvic organ prolapse. This can reveal itself as a feeling of vaginal heaviness, the sensation that something is falling out vaginally, or being able to feel a bulge in the vagina. As noted above, we lose a significant amount of muscle mass after menopause. If this affects the pelvic floor muscles, then there is a loss of support for the pelvic organs. This, combined with straining to empty your bowel, heavy lifting, a history of difficult childbirths (forcep deliveries, prolonged 'pushing' to birth the baby etc) and/or abdominal weight gain can lead to a prolapse developing or worsening.
In addition, the drop in oestrogen affects the non-stretch supporting tissues of the pelvis which can also lead to a prolapse developing or worsening.
The Pelvic Health Physio Approach: It is rarely necessary for surgery to be the first step in management of a prolapse as there are good conservative (non-surgical) treatment options to relieve symptoms and prevent the prolapse getting worse:
Pelvic Floor Muscle Retraining: To optimise the dynamic support for the pelvic organs
Abdominal Pressure Management: The pressure inside the abdominal cavity is fluctuating all the time relative to our activities and movement (think about coughing, sneezing where the abdominals quickly brace, or physical activities where you're carrying load, or running, jumping). The pelvic floor muscles should be working automatically with the deep core muscles to 'contain' this pressure, however if they are not, the pressure can escape downwards putting pressure on the pelvic organs, potentially causing or exacerbating a prolapse. Learning how to move, lift, and breathe in coordination with the pelvic floor muscles can significantly counter these inceases in pressure, minimise your symptoms and stop the prolapse from getting worse.
Vaginal Support Pessaries: These are internal silicone supports. Think of them like an ankle brace that instead of being worn externally around the joint, is worn internally in the vagina to support the organs. They can be used for the long term and are an excellent way to avoid surgery. There are many different kinds of pessaries that we fit depending on what kind of prolapse you have and how severe it is. They come in different sizes so that the fitting can be individualised to your needs.
For more information on pelvic organ prolpase, watch our video "What is a Prolapse" and/or read our blog "Pelvic organ prolapse (POP)"
Menopause Health Essentials
Taking a proactive approach throughout peri-/post-menopause is vital because many changes can be "silent."
Focusing on the following core areas will help you to protect your long-term wellbeing:
Understand Your Hormones: Talk to a GP who understands how hormones affect you both across your whole body (systemic) and within the pelvis (local). This allows for a nuanced discussion around Menopause Hormone Therapy (MHT) - previously known as hormone replacement therapy.
Have a pelvic health check up with a Pelvic Health Physio: They will discuss all your symptoms and concerns with you at length then formulate an individually tailored plan to address them.
Optimise Your Exercise: High-load strength training is essential for building bone and muscle mass. Additionally, PFMT improves local blood flow and tissue quality.
Consider Your Nutrition: Prioritise high-quality protein to preserve muscle mass and ensure adequate Calcium and Vitamin D for your bones.
Refine Your Lifestyle: Aim to ensure a healthy sleep pattern, minimise stress and alcohol, eat well and maintain a regular exercise routine. These all help to control your symptoms.

In Summary
Although there are a multitude of changes that occur in our lives when we go through the journey that is menopause, some of which really negatively impact our quality of life, there are now many options to help manage this. One of these options is seeing a Pelvic Health Physio. At Beaches Pelvic Physio we have 6 experienced Pelvic Health Physio's who regularly treat women with symptoms of menopause including painful sexual intercourse, bladder/bowel issues and prolapse symptoms, with great outcomes so please feel free to get in touch with us to find out more.
References
British Menopause Society (BMS) (2025). Consensus Statement on Genitourinary Syndrome of Menopause (GSM). Published online November 2025. BMS Official Publication
El Khoudary, S. R., et al. (2020). Menopause Transition and Cardiovascular Disease Risk: Implications for Timing of Early Prevention: A Scientific Statement From the American Heart Association. Circulation, 142(25), e506–e532. DOI: 10.1161/CIR.0000000000000912
Gandhi, J., et al. (2016). Genitourinary syndrome of menopause: an overview of clinical manifestations, diagnosis, and management. American Journal of Obstetrics & Gynecology, 215(6), 704–711.DOI: 10.1016/j.ajog.2016.07.045
Mercier, J., et al. (2023). Pelvic floor muscle rehabilitation for genitourinary syndrome of menopause: why, how and when? Climacteric, 26(4), 302–308. DOI: 10.1080/13697137.2023.2194527
Rueda, C., et al. (2017). The efficacy and safety of estriol to treat vulvovaginal atrophy in postmenopausal women: a systematic literature review. Gynecological Endocrinology, 33(10), 747–754. DOI: 10.1080/09513590.2017.1329291
USANZ (2024). Submission to the Australian Senate Inquiry into Issues Related to Perimenopause and Menopause. Provided by Dr Sandra Elmer. Link: USANZ Official Submission
Wright, A., et al. (2024). The musculoskeletal syndrome of menopause. Climacteric (Journal of the International Menopause Society), 27(5), 415–421. DOI: 10.1080/13697137.2024.2380363

Comments